Vertigo is a sensation of spinning or dizziness that can make daily activities challenging and, at times, debilitating. While many people associate vertigo with inner ear issues, not all vertigo originates from the same source. It can broadly be classified into two categories: central vertigo and peripheral vertigo. Understanding the differences between these two types is crucial for accurate diagnosis and effective treatment, especially when applying a functional neurology approach.
Peripheral Vertigo: Inner Ear Disorder
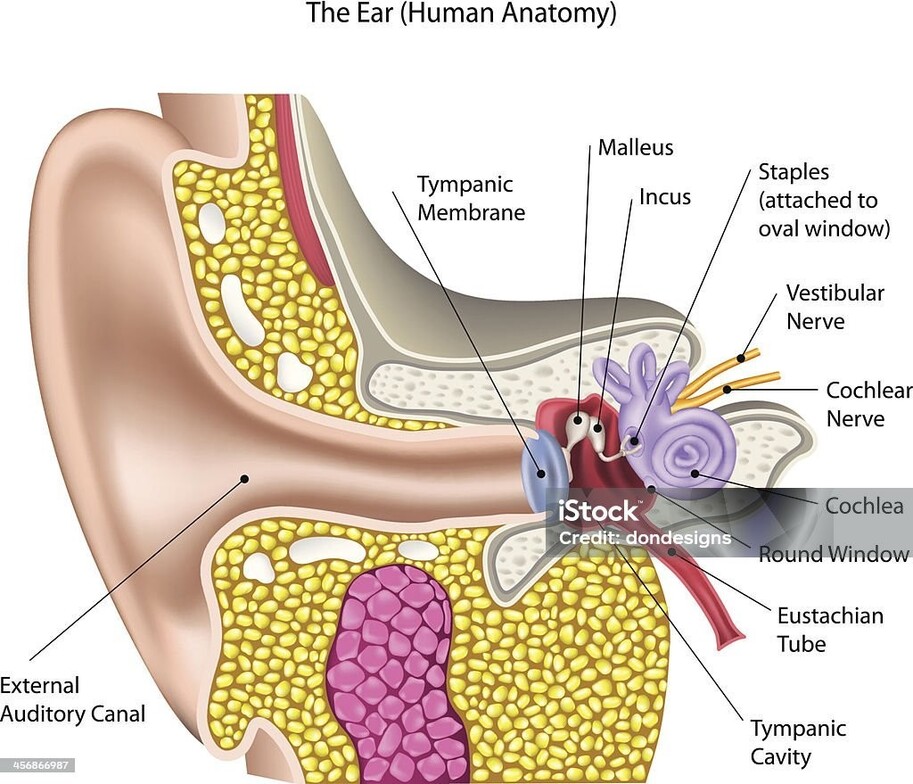
Definition: Peripheral vertigo is the most common type of vertigo and is caused by dysfunction in the inner ear or the vestibular nerve, which connects the inner ear to the brain. The inner ear plays a critical role in maintaining balance, and any disruption in this system can lead to dizziness and imbalance.
Causes:
-
Benign Paroxysmal Positional Vertigo (BPPV): Tiny crystals made of calcium, called otoconia, break off of membranous structures within the otolith and float into the semi-circular canals of the inner ear, causing abberrant signaling to the brain that make it feel like you are spinning.
-
Meniere’s Disease: Also called endolymphatic hydrops, is condition characterized by fluid buildup in the inner ear, leading to vertigo, tinnitus, and hearing loss.
-
Vestibular Neuritis: Inflammation of the vestibular nerve, often due to viral infections.
-
Labyrinthitis: Inflammation of both the inner ear and the vestibular nerve.
Symptoms:
-
Intense spinning or dizziness, often triggered by head movements.
-
Nausea and vomiting.
-
Tinnitus (ringing in the ears) or hearing loss.
-
Difficulty maintaining balance.
Functional Neurology Perspective: Functional neurology addresses peripheral vertigo by identifying the specific dysfunction within the vestibular system. Through a combination of precise vestibular assessments and neuro-rehabilitation techniques, such as canalith repositioning maneuvers and gaze stabilization exercises, the root cause of symptoms can often be corrected.
Central Vertigo: A Brain-Based Issue
Definition: Central vertigo originates from dysfunction in the central nervous system (CNS), particularly the brainstem or cerebellum, which are responsible for processing balance and spatial orientation.
Causes:
-
Stroke or Transient Ischemic Attack (TIA): Reduced blood flow to the brain can impair balance centers.
-
Multiple Sclerosis (MS): Inflammatory damage to nerve cells can affect the brain’s ability to process balance signals.
-
Vestibular Migraine: Vertigo associated with migraine headaches.
-
Brain Tumors: Pressure or damage to the balance centers in the brain.
-
Traumatic Brain Injury (TBI): Damage to the brainstem or cerebellum.
Symptoms:
-
Gradual onset of dizziness or unsteadiness.
-
Imbalance that is less positional and more persistent.
-
Neurological symptoms such as double vision, difficulty speaking, or weakness.
-
Typically less severe nausea compared to peripheral vertigo.
Functional Neurology Perspective: For central vertigo, functional neurology focuses on identifying the neurological pathways affected. A detailed evaluation of eye movements, coordination, and sensory integration helps uncover deficits. Targeted neuro-rehabilitation exercises, such as vestibular stimulation, visual-motor training, and neuroplasticity-based protocols, aim to retrain the brain’s balance centers and restore function.
Diagnosing Vertigo
Proper diagnosis is essential for effective treatment. Functional neurology employs advanced tools and techniques to assess both peripheral and central vertigo. A thorough clinical evaluation typically includes:
-
Medical History: To identify potential triggers, such as infections, trauma, or migraines.
-
Physical Examination: Assessment of balance, coordination, and eye movements.
-
Specialized Tests:
-
Dix-Hallpike and Eply maneuvers for BPPV.
- Videonystagmography (VNG) to identify central nervous system pathology and evaluate eye movements.
-
Imaging studies (MRI or CT scan) to rule out central causes.
-
Sensory and motor testing to identify underlying neurological dysfunction.
-
Treatment Approaches
Peripheral Vertigo:
-
Functional Neurology Techniques: Canalith repositioning maneuvers, gaze stabilization, and customized vestibular exercises.
-
Lifestyle Modifications: Reducing salt intake or managing stress, modifying sleeping position.
Central Vertigo:
-
Functional Neurology Rehabilitation: Customized programs using neuroplasticity-based exercises, balance training, and coordination drills to restore proper brain function.
-
Addressing Underlying Conditions: Treatment for TBI, stroke, MS, or migraines.
Functional neurology offers a comprehensive and patient-centered approach to managing both central and peripheral vertigo. By targeting the root cause of symptoms through tailored neuro-rehabilitation strategies, patients can achieve lasting relief and improved quality of life. If you experience persistent or severe vertigo, give us a call today!

Benjamin Pupo
Contact Me

.jpg)

